Introduction
The use of inositols in clinical practice is closely related to PCOS or polycystic ovary syndrome, an endocrine-metabolic disorder widespread among women of childbearing age and with serious consequences for women’s health. Suffice it to say that PCOS among women is the leading cause of anovulatory infertility [1]. Although widespread, the treatment of PCOS still remains a challenge.
Currently, among the most used therapies are the birth control pill and, although there is no specific indication by the Ministry of Health and AIFA, metformin.
However, the latter can produce significant side effects such as nausea, vomiting and gastrointestinal disturbances [2].
The poor compliance observed with metformin has prompted clinicians to seek new approaches for PCOS. The study of inositols in the context of PCOS stems precisely from the desire to find an alternative, effective and safe therapeutic response!
Let’s see together, starting from what is PCOS, what are the results achieved with inositol.
PCOS, what is it?
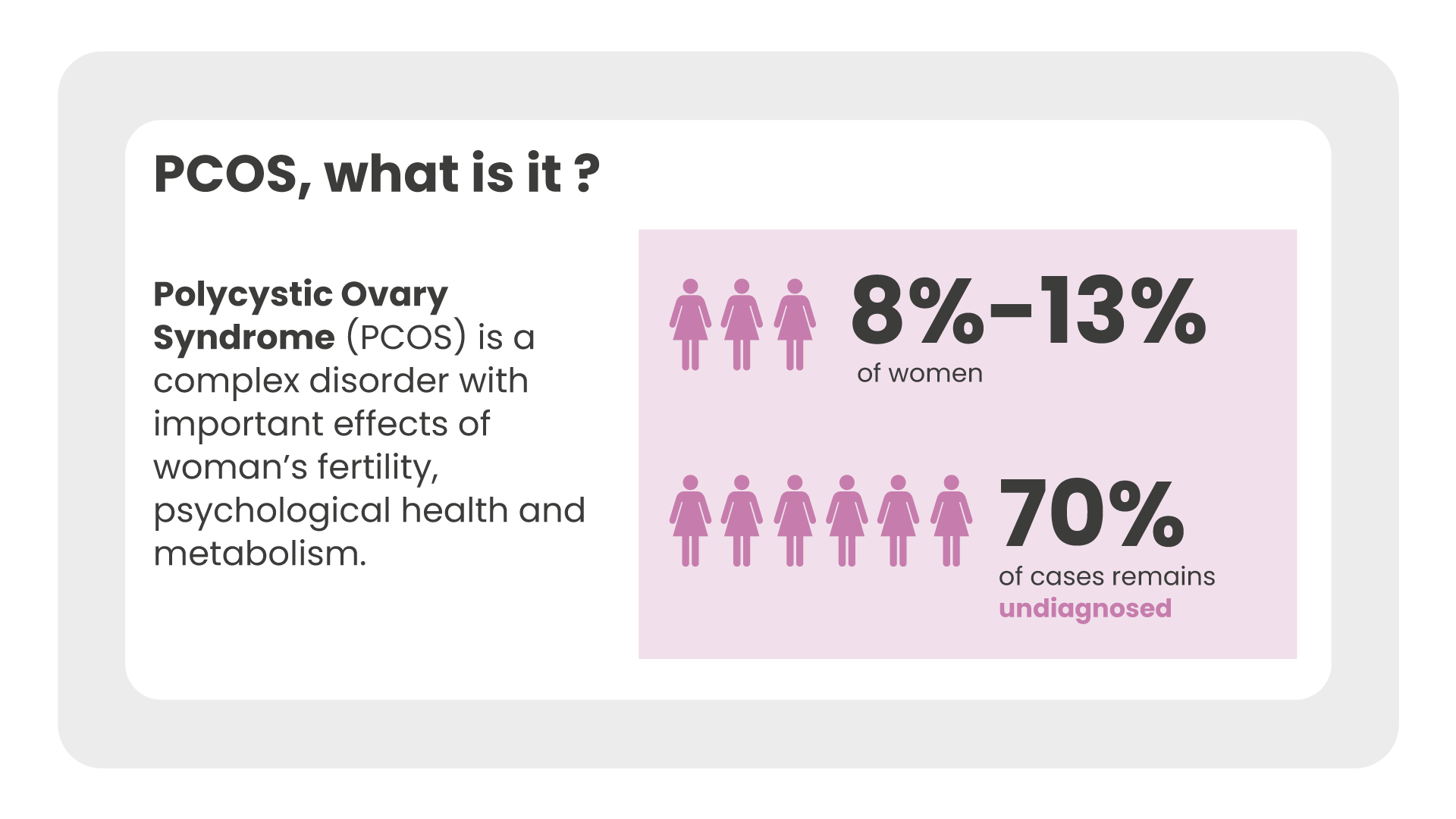
Polycystic ovary syndrome (PCOS) is a complex disorder with important effects on a woman’s fertility, her psychological health and metabolism.
It is a fairly common syndrome among women of childbearing age. According to the latest data reported by the ESHRE (European Society of Human Reproduction and Embryology), this affects between 8% -13% of women, while up to 70% of cases remain undiagnosed [3].
Signs and symptoms of PCOS
PCOS is a heterogeneous syndrome. Women who suffer from it have different characteristics:
- psychological disorders (anxiety disorders, depression);
- infertility (irregular menstrual cycles);
- signs of hyperandrogenism (alopecia, hirsutism, visceral fat);
- metabolic disorders (insulin resistance, metabolic syndrome, prediabetes, type 2 diabetes and cardiovascular risk).
Diagnosis and treatment
The diagnosis and treatment of PCOS still represent a challenge today, precisely because of the complexity and heterogeneity with which it occurs.
This diversity has led academics and researchers to identify four types (or phenotypes) of women with PCOS. In this regard, the Rotterdam criteria of 2003 [3] laid the fundamental foundations and guidelines for the diagnosis of PCOS and for the distinction of the four types.
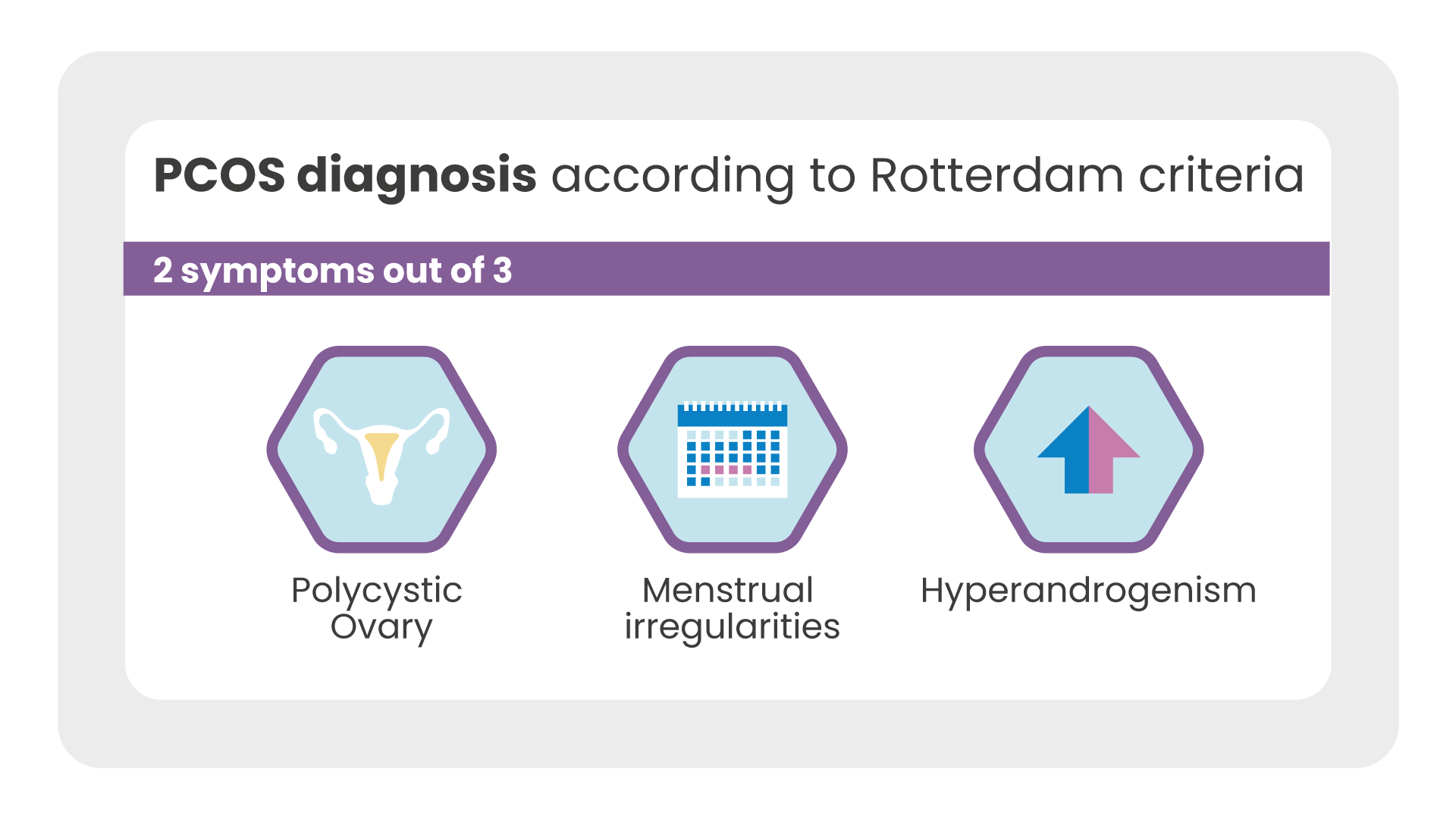
These establish that, to make a diagnosis of PCOS, the woman must have at least 2 out of 3 symptoms among them:
- multifollicular or polycystic ovary;
- menstrual cycle disorders;
- signs of hyperandrogenism.
Depending on the presence of these signs and symptoms, four types of PCOS can be identified:
- Phenotype A: hyperandrogenism + ovulatory dysfunction + polycystic ovary
- Phenotype B: hyperandrogenism + ovulatory dysfunction
- Phenotype C: hyperandrogenism + polycystic ovary
- Phenotype D: ovulatory dysfunction + polycystic ovary
Insulin resistance
In addition to the signs and symptoms listed above, it is good to remember that women with PCOS can present and, in most cases, present insulin resistance and metabolic disorders, even if these have not been included within the Rotterdam criteria.
In fact, among PCOS women, about 30% -40% of normal weight women and about 80% of obese women have insulin resistance [4].
What are inositols
Inositol is actually a group of 9 different stereoisomers, so it would be more correct to speak of “Inositols” in the plural.
Among these, myo-inositol and d-chiro inositol are the most important for the body’s physiological processes.
Myo-inositol is involved in the activation of transporters and the use of glucose, while D-chiro is mainly involved in the synthesis and storage of glycogen
The differences between the two molecules were investigated and studied in depth in an attempt to find a non-pharmacological therapeutic response to PCOS.
Both are able to act as second messengers of insulin.
As said before, that insulin resistance is a recurring trait in women with PCOS, regardless of weight.
Inositol metabolism in women with the syndrome is impaired. More specifically, in PCOS women there is an imbalance between myo-inositol and D-chiro inositol, to the detriment of the former.
Myo-inositol is also the second messenger of FSH, the follicle-stimulating hormone. In fact, many studies have shown how the integration of myo-inositol is able to improve the metabolic and hormonal parameters of women with PCOS, with benefits on the menstrual cycle and oocyte quality [5].
The results obtained by the integration of only d-chiro-inositol in PCOS at high dosages and for prolonged periods of time remain controversial [6].
To learn more read the article: Differences between inositol, myo-inositol and D-chiro-inositol
The benefits of myo-inositol in PCOS
Several clinical studies have shown how the constant intake of myo-inositol is able to restore both ovarian and metabolic function [7], [8].
A recent meta-analysis [7], which examined a series of studies involving a total of 496 women (including 247 with PCOS treated with myo-inositol and 249 controls), has shown that treatment with Myo-inositol significantly decreases the levels of insulin, HOMA-index and androgens (free testosterone), while increases those of sex hormone binding globulin (SHBG).
Previously, another Review [8] had provided evidence that myo-inositol significantly improves the rate of ovulation and regulates the frequency of menstrual cycles.
To learn more read the article: Myo-inositol: the benefits for PCOS
Myo-inositol: when, how much and why
Studies have shown the efficacy of myo-inositol in treating PCOS with the intake of 2g, twice a day (for a total of 4g) for the powder formulations (sachets, tablets).
In addition to the importance of dosages, studies highlight two other key elements for the effectiveness of myo-inositol.
- the intake, for the powder formulations, away from meals in order not to interfere with their absorption;
- repeated administration throughout the day.
Kinetic studies have shown a 12-hour half-life of inositol [9]. By using double administration, better coverage of the insulin response is obtained.
However, research has raised some concerns about the use of D-chiro-inositol at high dosages and for prolonged periods with a potential negative effect on the quality of blastocysts [6].
To learn more read the article: D-chiro inositol: what it is, use and benefits
The ovarian paradox in PCOS
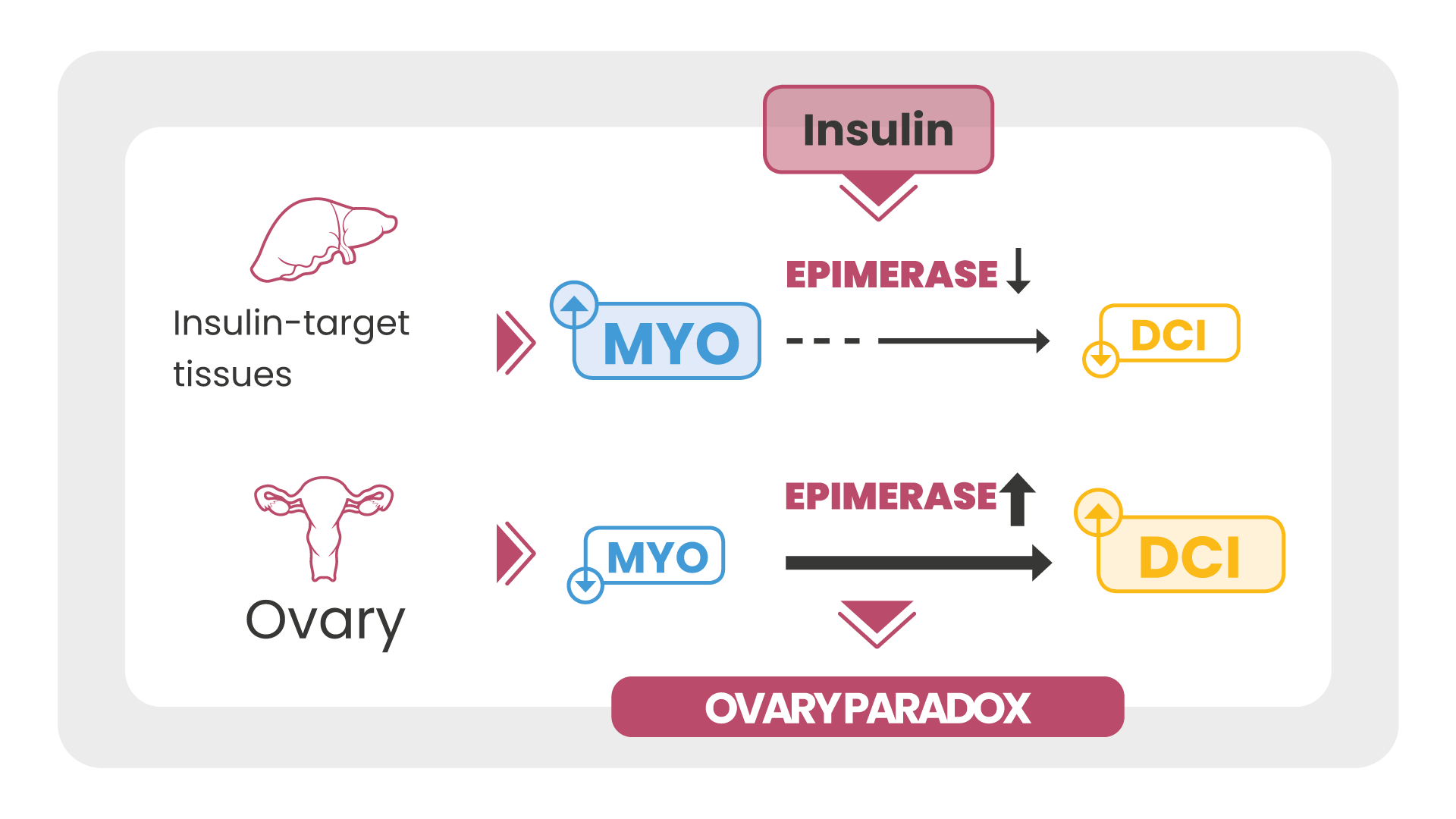
For the purpose of treating PCOS what is important to know is that in women suffering from this condition, there is a deficiency of myo-inositol and an excess of D-chiro in the ovarian level.
This mismatch is due to the excessive activity of an enzyme, epimerase which depends on insulin and which regulates the conversion of myo-inositol to D-chiro-inositol.
The insulin resistance of PCOS women generates hyperinsulinemia. The body’s cells are practically “deaf” to the insulin signal and the body responds by producing more and more.
However, the ovary is never insulin resistant. In PCOS women, epimerase is overstimulated by the insulin signal, causing an excessive conversion of Myo to D-chiro inositol. In the PCOS woman the ovary becomes rich in d-chiro and deficient in myo-inositol, with a negative effect on the FSH signal and on the oocyte quality [10].
To learn more read the article: D-chiro-inositol: what it is, use and benefits
Myo and D-chiro 40:1
In a clinical study of 46 obese PCOS women, a combined therapy of Myo and D-chiro inositol was administered in the 40:1 ratio (in other words a treatment mainly based on myo-inositol and only a small part of d-chiro ) for 6 months.
The study authors noted that:
- insulin sensitivity had improved;
- improvement of ovulation;
- a decrease in LH and free testosterone;
- a significant reduction in the HOMA index.
In short, the study showed an improvement in hormonal, metabolic and ovulation parameters without side effects [11].
To learn more about this topic go to the section: The true story of MYO and D-Chiro 40:1
Sources
[1] The Role of Polycystic Ovary Syndrome in Reproductive and Metabolic Health: Overview and Approaches for Treatment, Carrie C. Dennett and Judy Simon, 2015
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4433074/
[2] Facchinetti, F, et al. Short-term effects of metformin and myo-inositol in women with polycystic ovarian syndrome (PCOS): a meta-analysis of randomized clinical trials. Gynecological endocrinology, 2019. https://doi.org/10.1080/09513590.2018.1540578.
[3] International evidence-based guideline for the assessment and management of polycystic ovary syndrome (PCOS), European Society of Human Reproduction and Embryology (ESHRE), 2018
https://www.monash.edu/__data/assets/pdf_file/0004/1412644/PCOS_Evidence-Based-Guidelines_20181009.pdf
[4] Baillargeon, JP & Iuorno, MJ & Nestler, JE. (2003). Insulin Sensitizers for Polycystic Ovary Syndrome. Clinical Obstetrics and Gynecology. 46. 325-340. 10.1097/00003081-200306000-00011.
[5] Antonio Simone Laganà, Inositol in Polycystic Ovary Syndrome: Restoring Fertility through a Pathophysiology- Based Approach, Cell Press, 2018
[6] Can high levels of D-chiro-inositol in follicular fluid exert detrimental effects on blastocyst quality? Eur Rev Med Pharmacol Sci K. Ravanos, G. Monastra, T. Pavlidou, M. Goudakou, N. Prapas, 2017
[7] Unfer V. Et al. Myo-inositol effects in women with PCOS: a meta-analysis of randomized controlled trials. Endocr Connect. 2017 Nov;6(8):647-658
[8] Pundir et al. Inositol treatment of anovulation in women with polycystic ovary syndrome: a meta-analysis of randomised trials. BJOG. 2018 Feb;125(3):299-308.
[9] Monastra et al. Alpha-lactalbumin effect on myo-inositol intestinal absorption: in vivo and in vitro. Curr Drug Deliv. 2018;15(9):1305-1311.
[10] Unfer V, Carlomagno G, Papaleo E, Vailati S, Candiani M, Baillargeon JP. Hyperinsulinemia Alters Myoinositol to d-chiroinositol Ratio in the Follicular Fluid of Patients With PCOS. Reprod Sci. 2014;21(7):854-8
[11] Benelli E, Del Ghianda S, Di Cosmo C, Tonacchera M. A Combined Therapy with Myo-Inositol and D-Chiro-Inositol Improves Endocrine Parameters and Insulin Resistance in PCOS Young Overweight Women. Int J Endocrinol. 2016;2016:3204083.
Other topics that may interest you
Myo-inositol
D-chiro-inositol
40:1
Alpha-lactalbumin
Overweight